Eva Mary Giles
 Eva was the perfect daughter – beautiful, funny, feisty and fun. She was the ultimate girl – into anything princess related, pink, glittery, loved her clothes and dressing-up. She was very caring and tuned into other people’s emotions. Eva had the personality that tied all our children together, with a six year age gap between oldest and youngest, Eva was perfectly placed to bring them all together. She was often the instigator of games. Usually her games were role-playing with a host of soft-toys as her audience.
Eva was the perfect daughter – beautiful, funny, feisty and fun. She was the ultimate girl – into anything princess related, pink, glittery, loved her clothes and dressing-up. She was very caring and tuned into other people’s emotions. Eva had the personality that tied all our children together, with a six year age gap between oldest and youngest, Eva was perfectly placed to bring them all together. She was often the instigator of games. Usually her games were role-playing with a host of soft-toys as her audience.
Eva was defined by her laugh, so loud and honest, it was difficult to tell sometimes if she was screaming or laughing!! She loved jokes and had already began to develop a very cheeky sense of humour.
Eva was a force of nature, and unbelievably strong minded for her age. We were so proud of her for being the kind of person who did what she wanted, and on her own terms (Even though it made it difficult, at times, to parent her!!!).
She loved her siblings, older brother, Euan, and younger sister, Rosie, and they both miss her so terribly
Symptoms
Eva had suffered with night terrors for a year or so before we knew anything was seriously wrong. She’d often scream out in the night, was quite restless, by the time we’d jumped out of bed and got to her room she would be laughing in her sleep. It seemed strange, but harmless enough at the time (this is a symptom related to DIPG, which we discovered after diagnosis).
In the months leading up to Eva’s diagnosis she had become insecure about being left at school, and uncharacteristically nervous about going down stairs on her own. At a party in December 2015, four months before diagnoses, she was nervous about playing on the bouncy castle with other children, and was reluctant to join in party games. This was not normal behaviour for Eva.
In March 2016 it became obvious she wasn’t hearing well. In the following weeks her face started to droop on one side when she was laughing or crying, her walking became unsteady, and she started to lose balance and use walls to steady herself. Her right leg collapsed beneath her a few times. For me, the most alarming symptom was when her head started to tilt to the side
 Last Spring we watched in disbelief as Eva’s body slowly failed her. At first the signs were subtle, her smile became crooked. Then she was falling over more, and her right leg seemed to have a mind of its own. She appeared to be leading with one side of her body. GP after GP failed to see how seriously ill she was. we were forced to visit the GP surgery three times, and the A&E department twice. All doctors showed a complete inability to recognise these extremely worrying symptoms. Despite a lost (un-urgent) referral letter from the GP to the hospital, and through hard work on my part phoning between hospital and GP surgery, I finally managed to get a specialist appointment. It was, at this point, nearly too late.
Last Spring we watched in disbelief as Eva’s body slowly failed her. At first the signs were subtle, her smile became crooked. Then she was falling over more, and her right leg seemed to have a mind of its own. She appeared to be leading with one side of her body. GP after GP failed to see how seriously ill she was. we were forced to visit the GP surgery three times, and the A&E department twice. All doctors showed a complete inability to recognise these extremely worrying symptoms. Despite a lost (un-urgent) referral letter from the GP to the hospital, and through hard work on my part phoning between hospital and GP surgery, I finally managed to get a specialist appointment. It was, at this point, nearly too late.
With the increase of worrying symptoms, I booked an emergency GP appointment. Upon listening to the symptoms, and briefly checking her over, the GP diagnosed impacted earwax and sent us away with olive oil eardrops!! Over the next two days, her symptoms worsened, so I took her back to the GP, and this time saw the Ear Nose and Throat specialist. He was sure it wasn’t ears related. However, as Eva didn’t have any headaches or vomiting, he didn’t feel it was necessary to treat as urgent, and chose to refer her for further assessment at the local hospital at a later date.
A week later we still had no referral date, and with Eva’s symptoms continuing to worsen, we made the decision to take her to A&E at our local hospital, QEQM in Margate. After a long wait we were taken to the paediatric ward. A doctor’s examination warranted a second opinion. More waiting, and by then we had been in the hospital for several hours. Eva became very uncomfortable and vomited in the waiting room. They lay her on a bed where she lay unresponsive with her eyes rolling back into her head (a symptom of DIPG). Once the paediatric doctor arrived, he read the notes, asked me about the GP’s diagnosis, and sent us home with more olive oil, and further advice to visit the GP again on Monday!
Over the weekend our concern for her rose to desperate alarm, and we considered going back to A&E, but felt we would be sent away again and didn’t want to put Eva through the hours and hours of waiting again so soon. Instead, we decided to wait until Monday, we booked a third GP appointment again once again listed her symptoms. After her examination, the doctor tried to get through to the paediatric department at QEQM on the phone. She held the line for ten minutes before giving up and instructed us to go straight to the hospital in Ashford, where they have a specialised ear, nose and throat department.
It didn’t feel right. By this point we were incredibly worried about her and an ear problem didn’t ring true. We took the decision instead to chase the referral letter. I rang the hospital in Canterbury and was told there was no referral letter in the system. I then went back to the doctor’s receptionist who clarified the letter had been lost, and she would resend over to QEQM in Margate. (lost referrals became part and parcel of the process at all levels of the NHS, we found, over and over, that if you do not chase referrals there’s a high chance it will not find it’s destination).
As soon as they received the letter, they called us with an appointment the following day – Tuesday 12th April. I took her to QEQM that morning and was seen by a paediatric consultant. After performing a number of neurological tests, and asking health related questions, he told me he was ‘very concerned’ about Eva and would need to admit her as an in-patient for an MRI scan, then further tests if necessary.
I felt sick to the pit of my stomach.
 Diagnosis
Diagnosis
The doctor arranged an emergency MRI on the Thursday in Canterbury. They sent us home Wednesday evening and told us to be at Canterbury early the next day. That was the day that our lives changed forever.
We arranged babysitters for our other children and together we took Eva that morning. The MRI went as planned, but there was a distinct change in the way the staff were handling us. QEQM booked an ambulance for us (Eva and Emma) and took us quickly, with blue lights flashing, back to QEQM. Dean met us there. The Doctor took us through to a meeting room with a small table in the middle and a box of tissues placed neatly on top. In the room there were a couple of nurses and woman with a clipboard. Everything else is blurry. I remember the words ‘lesion’ in a part of the brain that was a ‘problem’….and I sat there numb unable to find tears. Dean cried uncontrollably beside me, as did Eva’s nurse.
I went back to Eva, and made necessary phone calls to family while in a state of shock. It was a whirlwind of activity with phone calls, text messages, panicking family members…. all while Eva lay on a hospital bed watching Team Umizoomi on her ipad. QEQM were in contact with London hospitals to see where she would be cared. The doctors placed her on a high dose of steroids (dexamethasone) to help with brain swelling, and symptom management.
That day, QEQM informed us that The Royal Marsden in Sutton would take over her care. Royal Marsden gave us an appointment for Monday 18th April, and they booked an ambulance for early Monday morning. At this point she had not been officially diagnosed, all we knew was that she had a brain tumour. The details of what kind or it’s location were kept from us until we saw the Royal Marsden team. It was Thursday, and we had to wait until Monday for our appointment.
To say the wait was difficult would not do it justice. I look back on those days with a feeling of deep dread. Those four days of waiting, with no idea of the prognosis, while we watched our little girl fade away before our eyes, was like being in hell.
Monday 18th April eventually came. Eva was very scared about being taken to another hospital, but we tried to reassure her that it was the best thing for her.
The Royal Marsden immediately took her for a CT scan, and we were seen soon after by our new oncologist. We entered the room and were immediately confronted with five or six people – all of whom would become part of our lives over the next year as they all played a part in Eva’s care.
We were told that this tumour is ‘very serious,’ that she would be starting radiotherapy (13 sessions) the next day. The tumour is inoperable, it sits in the area of the brain known as the pons, and there is no cure. The tumour is likely to grow back within a year after radiotherapy. They told us there is 0% to 1% chance of survival beyond five years, but some of those statistics may have been misdiagnosed, making it almost certain that she will die.
We asked if there were medical trials available. Yes, but highly experimental and unproven. They recommended we don’t re-mortgage our house and fly over to America!
Again, I couldn’t process any of this information properly. None of it made any sense. How is my perfect, healthy four year old daughter, who has just started school and is planning her 5th birthday party, now sitting here with an inoperable brain tumour, for which there is no cure. This is 2016 – how can there be no cure?
Later, once we arrived back home we opened a folder containing emergency contact details listed for us. Here we saw the name of the tumour for the first time: DIPG (Diffuse Intrinsic Pontine Glioma).
A few days later Dean started to research online, a full three weeks before I had the courage. Being unprepared for what we found online is a huge understatement. We were confronted with the raw, bare facts – 0% survival, 9 months average survival from diagnosis, average age 5-9, 30-40 kids in the UK diagnosed every year – NO long term survivors – NONE.
Our oncologist, a highly respected and caring man with a wealth of experience, very carefully, and very deliberately, explained to us the results of the MRI. The tumour is located in the pons, an area of the brain that controls critical functions like movement and breathing. It is located in the brainstem and therefore inoperable. He offered us no hope – Eva was likely to die within a year.
She would start radiotherapy the following day, and if we were lucky, that would give us a few more months. Every single child diagnosed with DIPG so far has died. A sad and terrible fact.
On the other hand, the Consultant advised us and fully supported our decision to try experimental treatments. Without his help we would have been blind in those early days.
Due to the delay in Eva’s diagnoses, by the time she started radiotherapy she could barely swallow, talk or walk. She’d lost all of her ‘spark’ and was a frightened and clingy little girl. She sailed through radiotherapy, dealing with everything that was thrown at her, and considering her age she managed it all without sedation.
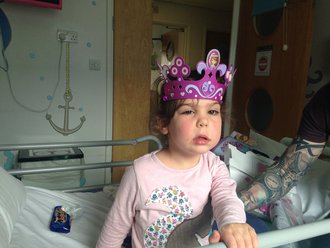 We started to see the effects very quickly. She started on the Tuesday, and already by that weekend she’d started to walk more, and was eating better. The steroids continued to change her appearance, which was very difficult – she went from being a petite, little girl to overweight and bloated. When she thought we weren’t looking, she would sit in front of the full length mirror in our bedroom lifting her droopy eye up so it matched the other. Just one of the many heart-breaking moments.
We started to see the effects very quickly. She started on the Tuesday, and already by that weekend she’d started to walk more, and was eating better. The steroids continued to change her appearance, which was very difficult – she went from being a petite, little girl to overweight and bloated. When she thought we weren’t looking, she would sit in front of the full length mirror in our bedroom lifting her droopy eye up so it matched the other. Just one of the many heart-breaking moments.
Despite this she was determined to make the best of things, and even managed a few days at school once the treatment had finished.
During the radio therapy, we felt a false sense of security – despite knowing that radiotherapy is palliative care, you still feel like you are doing something to fight the tumour. Once the treatment had finished we felt very lost. We started searching everywhere, and contacting doctors all over the world. We would do absolutely everything in our power to save our little girl. The most promising treatment actually turned out to be in the UK. Using a delivery system called Convection Enhanced Delivery (CED) which is a method for delivering drugs directly to the pons area of the brain, therefore passing the blood brain barrier. We found a hospital in Bristol had been running a trial, and a couple of children were doing well – living past the expected survival time. The trial was no longer running, but they were able to take children on a compassionate basis, at a personal cost of £80,000. In the meantime, we had set up a social media page for Eva – a way of keeping friends and family up to date with her illness, and also linking in a fundraising account for friends and family to raise money to enable us to get her onto this method for treatment.
Eight weeks after finishing radiotherapy Eva had a follow up MRI. The results showed the tumour had reduced in size significantly, and her general clinical condition was improving. Our oncologist said she would be a good candidate for CED and the consequent drug infusions, and he would refer her to Bristol. As you can probably imagine, we glimmered the first ray of hope – this new technology at the cutting edge was an unknown at the time. When there is 100% failure rate in the DIPG world “new” means everything. However, Bristol closed the program and our budding hope was crushed. – just like that!
Bristol told us they were oversubscribed, and treating more children would negatively affect NHS patients.
We were shocked, furious, helpless….how can they refuse our child when we are offering them £80,000 and there is nothing else?! We would have paid double, triple that amount. There was light at the end of the tunnel, the compassionate care CED programme would reopen in six weeks. We desperately clung to that promise. Through researching and discussing our options with professionals and parents alike, we came to believe that treatment timing was just as important, perhaps more so, than the type of drug being used. Typically, DIPG would spread out of the pons and CED could only work while it remained contained in that area. Furthermore, CED can be likened to a sledgehammer approach, and the best time for the heavy hit is when the tumour is still reeling from the shock of radiotherapy. Crucially, before it has a chance to progress again.
We knew the longer we waited the less chance of success we had.
In the meantime, we booked a family holiday to center parks, Eva’s favourite place. Although still suffering with fatigue from the radiotherapy, Eva was determined to enjoy the holiday, and had started walking again very well. She was able to sit in a bike trailer with younger sister, Rosie, and play and swim almost as normal with both siblings.
We allowed the next six weeks to pass in a relatively normal way – Dean at work, Euan at school and Eva going into school on occasion. We continued to chase the Bristol team and were told time and time again it would be opening soon. Our oncologist was fully supportive, and understood our desperation.
It was getting to a point though, knowing that DIPG wouldn’t wait, that we felt we should look into other available treatments. Through social media we were able to follow other children’s journeys and track their treatment plans, and through this we investigated immunotherapy at IOZK clinic in Cologne. Again, this was “new” and although we felt it would be much better to use immunotherapy (specifically virotherapy), after we had hit the tumour with CED we knew this was better than doing nothing at all.
We contacted Dr. Stefan Van Gool at IOZK, and he kindly setup a skype meeting to discuss Eva’s condition, and how immunotherapy could help her. In an ideal world, CED should have been first, but we decided to pursue the treatment, fully aware that it wasn’t a cure, but knowing it might buy us valuable time. At a cost of more than 40,000 euros it took a lot to get us there, but on 26th July 2016 the whole family travelled over to Cologne by car, for 2 weeks. The plan at that point was to keep the tumour as stable as possible until CED re-opened, and we had a real chance at fighting this disease.
IOZK uses a virus that highlights the tumour to the body’s immune system, and uses the body’s natural defences to create a vaccine that in-turn bolsters the immune process. Eva endured a session every day, bar weekends, while we were in Germany.
She tolerated the immunotherapy treatment very well, in fact, with a cheeky smile on her face, and experienced very few side effects – the worst being a sore throat and slight fever. As much as was possible at the time, when even the happy moments were tinged with sadness, we enjoyed Cologne and met up with other families also fighting DIPG.
During this time it started to become clear that Bristol Hospital were having some problem. It transpired that no children were being treated by CED On contact they had discontinued the compassionate programme because there was not enough evidence of efficacy and they would continue only under trial condition. They simply would not help us.
We continued to fight for a place for our little girl. Dean contacted our local MP and kept up the dialogue with CED stakeholders.
We returned to Cologne again in August for three days, and September for three days. Things were going as well as they could, Eva was running around again, and had started to use her scooter, and we decided to book another family holiday in Center Parcs for the October half term, through the charity Make-A-Wish. It was Eva’s wish to go back to Center Parcs.
A week before going we noticed Eva was unstable on her feet again, and was crawling around on the floor rather than walking. The strength in her right was also becoming noticeably less again. We phoned the symptom team at The Royal Marsden and they said to start a course of steroids, if we felt necessary. In the meantime a doctor would call to discuss the onset of symptoms again.
We decided to go ahead with the trip anyway, but were becoming increasingly concerned that the original (before radiotherapy) symptoms were returning, and upon the advice of the doctor, she needed to have an MRI to rule out possible hydrocephalus. We only managed one day before we we had to leave center parcs for an emergency MRI. Our local hospital in Margate, QEQM, did everything they could to help. Everything with the MRI went as smoothly as possible. Eva woke from the sedation and we were able to go home soon after.
We waited an agonising week for the results. By this time, our oncologist had left NHS to work full time privately. He was now playing a pivotal role in the UK CED programme.
We met our new NHS oncologist a lovely and caring lady, and she explained that Eva’s tumour was, as we suspected, growing again.
By this point, the CED programme was moving from Bristol to Harley Street Clinic under the lead of our old Consultant, There are two parts to CED, firstly the operation to install the catheters that support the drug delivery. It is highly specialised requiring specialised surgeons and equipment. The catheters only need to be installed once, then they remain in the skull - semi-permanently.
The second part are the drug infusions.
At this point, I knew it was now or never for CED. It was already much later than we wanted to wait, and with progression becoming a reality, it really was our last chance.
Harley Street would have been able to oversee the second part of the process; he had the capability to infusion the drugs, all we needed was to have the operation, but the equipment was not ready! The MHRA needed to authorise its use in a new setting, which simply takes time.
We continued to push Bristol Hospital as they could still have operated on Eva at this point. They had the equipment, still gathering dust. why would they not do it? Bristol simply refused to help.
In the meantime, the Royal Marsden offered us a second round of radiotherapy. It had been six months past her last course, and she could receive another course of ten sessions. There were risks, of course, and this time more severe, and the percentage of the effect on the tumour was significantly less. Nonetheless, we decided to go ahead as Eva had responded so well the first time around, and we felt there were no other options.
The next few weeks became a blur again of hospital appointments – CT scans, radiotherapy treatments, physiotherapy, and speech and swallow tests…. Half way through the treatment, we became very concerned that either it might be causing swelling of the tumour, a common side effect, or it wasn’t having any effect at all.
Eva’s walking deteriorated, and she was very tired. After seeing a radiotherapy consultant we were advised to double the steroid dose, and hopefully the symptoms would subside. The steroids came with their own set of problems again – severe hunger, weight gain and mood swings. Our happy little girl once again became bloated and suffering with steroid rage.
We had to wait the standard eight weeks for an MRI, which was now being scheduled for December. In the meantime, our previous consultant, agreed that he would treat Eva as soon as the equipment was ready for use at Harley Street. He would need to see her latest MRI results and clarify she was still a candidate (i.e. that the tumour had not spread out of the pons). We were given a provisional date for surgery on 17th January 2017 – a full seven months after we started fighting for it (that’s seven months of an illness that has a nine month survival rate). Feeling as if we had some hope now, and secure in the knowledge that Eva had a surgery date. We duly booked the MRI and waited the obligatory seven days for the results.
The results were devastating. We received a phone call from and it was explained that the radiotherapy had worked in some areas of the tumour, but had not prevented it spreading out of the pons into the cerebellum. Eva was no longer a candidate for CED.
 We had desperately tried everything to get our daughter onto the only treatment showing any hope, been forced to wait eight months due to hospital politics, red tape and now what? Our innocent, beautiful, five year old daughter sitting in the back of the car playing, would lose her life to this deadly tumour. Did we have months, weeks or days?
We had desperately tried everything to get our daughter onto the only treatment showing any hope, been forced to wait eight months due to hospital politics, red tape and now what? Our innocent, beautiful, five year old daughter sitting in the back of the car playing, would lose her life to this deadly tumour. Did we have months, weeks or days?
By this time Eva was no longer walking, she was in a wheelchair and spending most of her days on the settee watching the TV. Her right foot was useless to her, locked in position.
Her eating and drinking was also becoming a struggle due to problems with swallowing. Despite all of this, she remained in high spirits, our happy gorgeous funny baby. She still enjoyed going out on day trips and breaking up the TV sessions with arts and craft activities.
At our follow up appointment at the Marsden we were delicately sent away with NO hope – there was no active treatment available for Eva, and no open clinical trials.
We didn’t want to give up, so we discussed other options available privately. It is much easier to have experimental treatment outside of the NHS, and after careful consideration we decided to try an oral drug combination that had shown some success in a medical trial in Milan, Italy. This was at a personal cost of £3,000 per month, with the intent of getting at least some of the drugs funded by the NHS – but the NHS wouldn’t take the risk of offering experimental drugs out of a trial setting. They actually recommended we did nothing and “make memories.”
F*** that.
Eva tolerated the drug combination relatively well, with few side effects. By March it was becoming difficult for her to lift her head so even sitting up became a problem. Her swallowing deteriorated, and her swallow reflex became very unresponsive. The drug combination didn’t appear to be working.
She caught a cold, and was too unwell to go through with a planned MRI beginning of March in London’s Harley Street. This would tell us if the drug combination had affected the tumour at all.
The doctors at Harley Street decided she was too unwell for the MRI. In fact, from the time we left home until we reached London, Eva had gone from feeling a bit wheezy to a full on chest infection. Her breathing was laboured and Harley Street ended up treating her with strong antibiotics. We didn’t anticipate the stay at Harley Street, and we were relieved that by 9pm that night they decided that she could go home.
By 8am the next morning things took a dramatic turn for the worse. Her breathing was noisy and laboured, she vomited and for the first time throughout all of this was crying out in fear and pain. This a moment that is entrenched in my mind. Dean was desperately trying to console her and keep her comfortable while I phoned 999. By this point, she started losing consciousness. The ambulance came within minutes, and everything moved quickly in a blur. She was hooked up to oxygen and taken by blue light to QEQM in Margate. Immediately taken into A&E where staff in blue scrubs rushed around trying to save our daughters life. She was sedated, hooked up to life support, and a consultant bellowed to me “has anyone discussed end of life care with you?” Which seemed really out of place and insensitive considering the circumstances.
Dean arrived, after settling the other two children with his parents, and the next few hours became a blur of watching and waiting. She looked so small on the bed… all the equipment and machines were designed for adults - how and why is this happening to her?
Chest x-rays revealed pneumonia. The consultant told us she needed a transferred to a London hospital with a paediatric intensive care unit, preferable St. Georges. By the afternoon, a mobile intensive care unit had arrived, and once again. Dean followed Eva and me in the ambulance to St. Georges. Again, I sat in the back of an ambulance with sirens blaring.
The journey took us to St. George’s hospital in Tooting. Doctors placed her in the isolation ward within the paediatric intensive care unit. The oral chemo had obliterated her immune system, and she was fighting a severe case of pneumonia. At this point all focus was on fighting the infection and we would worry about the tumour later.
Eva received amazing around the clock care at St. George’s, and they did everything in their power to save her. Her body was fighting the infection successfully, but she was not waking up after the sedation. It became slowly evident that the tumour was playing a role in her unconscious state. To be sure, the doctors ordered a CT scan that revealed huge tumour swelling.
The Royal Marsden symptom team visited us to discuss our options. What happened next was like living through diagnosis all over again. We’d travelled a full circle. Here we were, almost a year later to the day, sitting there discussing where our beautiful, loving, feisty, fun daughter was going to die. We had three choices, each involved turning the life support machine off, the choice was where it should happen: remain in hospital, be transferred to hospice, or go home. The choice was easy, she would want to be at home.
I took a final trip in the ambulance with my daughter, while Dean drove home ahead so he could deliver the impossible news to our other children. Family rallied around to say goodbye and 7th April 2017 our precious daughter lost her life to DIPG.
The day Eva died, Emma travelled home with her from the hospital in the ambulance, and I (Dean) drove back with a half-hour head start. I decided the quiet time before they arrived with an armada of doctors and nurses would be the best time to have “the” chat, explain to Eva's siblings that she would very soon pass away.
When I arrived home, Euan and Rosie were across the road in the park with their grandparents. It was a warm day for early April, and the sun was strong. I had known in the back of my mind this day would come, and I knew I’d have to have this conversation at some point, yet throughout the year of Eva’s illness I never once prepared what to say. If I had, it would have felt as if I was giving up on her. I took deep breathes and slowly walked over, my nerves tingling with each step.
I heard their voices first and fought with every ounce of my strength to stop from breaking down into tears. I felt it was important that I stay in control and explain things clearly and honestly. To do that, I needed to hold back my own feelings.
I took them to a quiet bench overlooking a large field and cricket pitch. The park was completely empty apart from us three, and Nan and Grandad keeping a respectful distance, but ready to help if I needed them. I hadn’t seen the kids for several days by then, and Rosie was confused and upset, wanting to cling on to me. I sat down, Rosie on my lap and Euan to my right. I explained about Eva’s infection, and how she had not been able to recover due to her brain tumour progression. I explained that she would be coming home so we could all say goodbye to her. I explained that she was going to die today.
I managed to get the basics across while I could still speak. Euan screamed for a moment and then very quickly recovered composure, which worried me. Euan and Eva were so close that I expected him to cry for hours. I later discovered that his reaction was fairly typical under these circumstances and it will take time for him to work through his emotions.
That was the second hardest moment of the day, and the third hardest moment of my life.
Why do you want to raise awareness of DIPG, and the importance of funding research into it?
In truth, I don’t want to. I wish with every part of me that I didn’t have to do this. Before Eva’s cancer journey, I had complete faith in the NHS and the supporting foundations that take care of us. As my family entered the world of DIPG, I realised quickly that my pre-conceived ideas were not just wrong, but utterly naïve. We entered a world where hardly any cancer research money goes to DIPG, yet DIPG kills up to forty of our children every year in the UK alone. And it is simply not newsworthy enough to be brought to the forefront of public awareness. Stop and think about that for a moment… forty children a year, that’s two classroom’s full of infant school age kids. These children are perfectly normal and happy, until one day they fall over. Gradually their bodies shut down, while maintaining complete cognitive awareness, they are fully awake as their legs and arms stop working. Gradually, they become locked-in, prisoner in their own shells – what could be worse for a fidgety energetic five year old? Their young healthy organs keeping them going for much longer than an adult’s would until finally they stop functioning. Our DIPG kids die a truly horrible death slowly over months. As parents, we watch every minute of it with desperation and helplessness. The reality of DIPG really is a living nightmare.
I don’t want to raise awareness because I don’t think we should have to. I think there should be more funds available for this deadly disease without people like us, people who’ve had their lives destroyed, having to bring it to the attention of government as a worthy cause.
However, here we are, having fallen through every crack in the NHS. Having to take a backseat to more newsworthy stories like gorillas being shot at a zoo, or a celebrity that cheated on her husband. A DIPG death rarely makes a front-page story. Perhaps if our kids were killed in a more alarming way, such as terrorism, perhaps then the government would take it more seriously.
Unfortunately, in our world, it’s not enough that our kids are dying, it’s how sensationally they die that warrants interest and awareness.
We navigate the world of DIPG and research treatment options ourselves, and find out the hard way that we are alone in our fight. Alone to self-fund for treatments, our only lifeboat, a few pioneering experts and other parents in our situation.
It’s a lonely path and more needs to be done to help future families.
I have followed research progress the past year, and researched what had come in the years before, and progress is being made. I think we will see a gradual improvement in mortality rates, and eventually this disease will become a chronic illness as opposed to a critical one. I only wish this could have happened while my daughter was alive, and I pray that other families and children do not have to tread the same lonely path we have.




